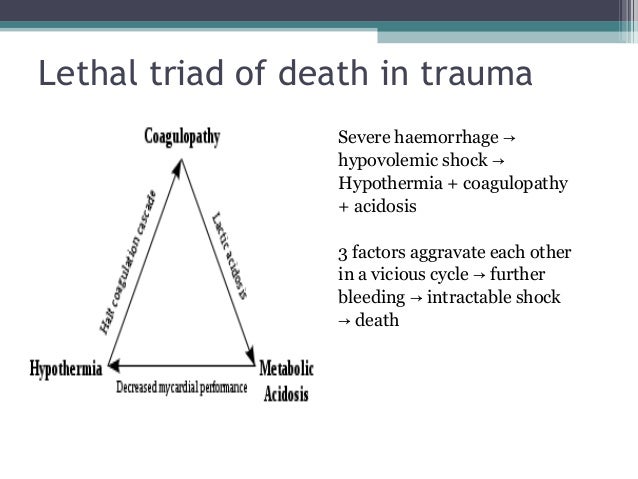
We know that the injury itself causes exposure of tissue factor (TF), which consequently causes thrombin and fibrin generation. Traditional doctrine suggests that coagulopathy associated with trauma results from consumption of clotting factors, in addition to the dilutional effects of resuscitation fluid. ( See Figure 1.) This cycle can be extremely difficult to break. Each factor compounds the other, leading to a worsening cycle and high mortality rate. The Lethal TriadĪ complex relationship exists between acidosis, hypothermia, and coagulopathy.

This concept revolves around the idea of rapid hemorrhage control through permissive hypotension, rapid correction of coagulopathy, acidosis, and hypothermia, in concurrence with damage control surgical techniques. Instead, the idea of damage control resuscitation has come into clinical practice. Traditional resuscitative efforts based upon aggressive fluid resuscitation with crystalloid to treat hypotension and tachycardia have fallen out of favor due to mounting evidence that they worsen coagulopathy, acidosis, and blood loss. There is mounting evidence that treating early coagulopathy in trauma patients improves survival.
TRAUMA TRIAD OF DEATH PLUS
Coagulopathy plus hypothermia and acidosis that occur in severe traumatic injury has been termed the "lethal triad" due to its high mortality. This coagulopathy is multifactorial, resulting from initial tissue injury and dilution and consumption of clotting factors and platelets. Traumatic injury requiring massive transfusion is associated with coagulopathy. 9 Postpartum hemorrhage is among the most common causes of maternal hemorrhage, with the majority of these cases due to uterine atony. 8 Obstetric hemorrhage has fallen from the first to the fifth leading cause of maternal death in the United States. Obstetric hemorrhage is the leading cause of maternal death worldwide and accounts for approximately 150,000 deaths annually. 6,7 As a result, hemorrhage necessitating transfusion of large amounts of blood products remains a major cause of potentially avoidable deaths. 5 Death from uncontrolled hemorrhage will typically occur within the first 6-12 hours following injury, and accounts for more than 50% of all trauma-related deaths that occur within the first 48 hours of hospital admission. 4 Yet, the mortality of patients who require massive transfusion ranges between 20% and 50%. 2 Massive transfusion is only required in 1-2% of civilian trauma patients 3 and in approximately 7% of patients in military settings. 1 In fact, traumatic injury is a leading cause of mortality and accounts for approximately 10% of all deaths worldwide. Traumatic injury continues to be the leading cause of death in people younger than the age of 40 worldwide. Although such subsets of patients require similar volumes of PRBCs, the need for other blood products may be variable. Historically, massive transfusion research has come from the trauma data however, hemorrhages as a result of gastrointestinal bleeding and obstetric and intraoperative emergencies are equally relevant. Massive transfusion is defined as a transfusion requiring greater than 10 units of packed red blood cells (PRBCs) in a 24-hour period. Patients with significant blood loss due to various etiologies, be it from trauma, ruptured ectopic pregnancy, or ruptured abdominal aortic aneurysm, are encountered in the emergency department (ED). Hypothermia should be avoided and treated when present, as it shifts the oxygen hemoglobin dissociation curve and worsens coagulopathy.It is now recommended that the blood pressure be allowed to be as low as 90 systolic if the patient has a normal mental status. Traditional resuscitation with large amounts of crystalloid leads to worsening coagulopathy, acidosis, and blood loss.The goal of resuscitation is to prevent or reduce these factors. After severe trauma with blood loss, the "lethal triad" of acidosis, coagulopathy, and hypothermia is associated with higher mortality.
